
The risk of death for dogs under anesthesia used to be one to two deaths in 100 patients, says Lois Wetmore, DVM, an assistant professor of anesthesia and pain management at the Tufts Cummings School of Veterinary Medicine. “Now we’re down to about one death in 2,000,” Dr. Wetmore says. “We’re headed in the right direction.”
Yet while anesthesia for dogs (and cats) has come forward by leaps and bounds, it lags behind anesthesia for people. Moreover, the veterinary community is right now in the midst of a crisis that is making it more challenging to keep pets out of pain when they undergo surgery or sustain a traumatic injury. Dogs are not alone. Anesthesiologists who treat people are facing the same crisis.
For a better understanding of the advances in anesthesia as viewed against current difficulties, we sat down with Dr. Wetmore, a board-certified veterinary anesthesiologist who treats dogs and other pets at Tufts’ Foster Hospital for Small Animals in addition to teaching veterinary students and conducting anesthesia research.
Your Dog: Why is it that dogs are so much safer under anesthesia now than they used to be?
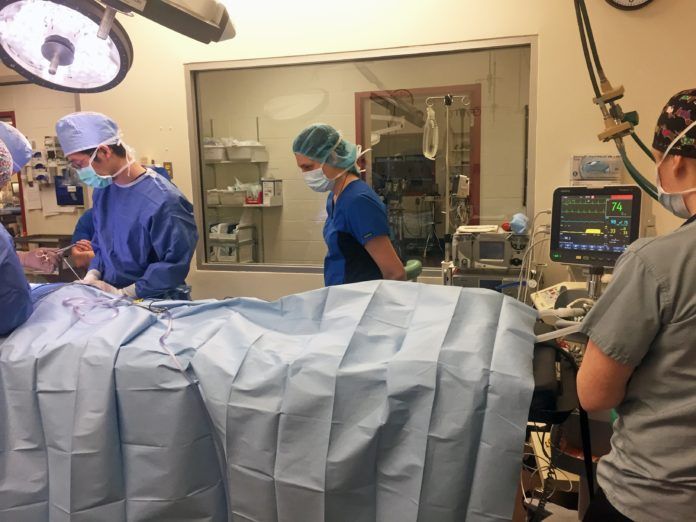
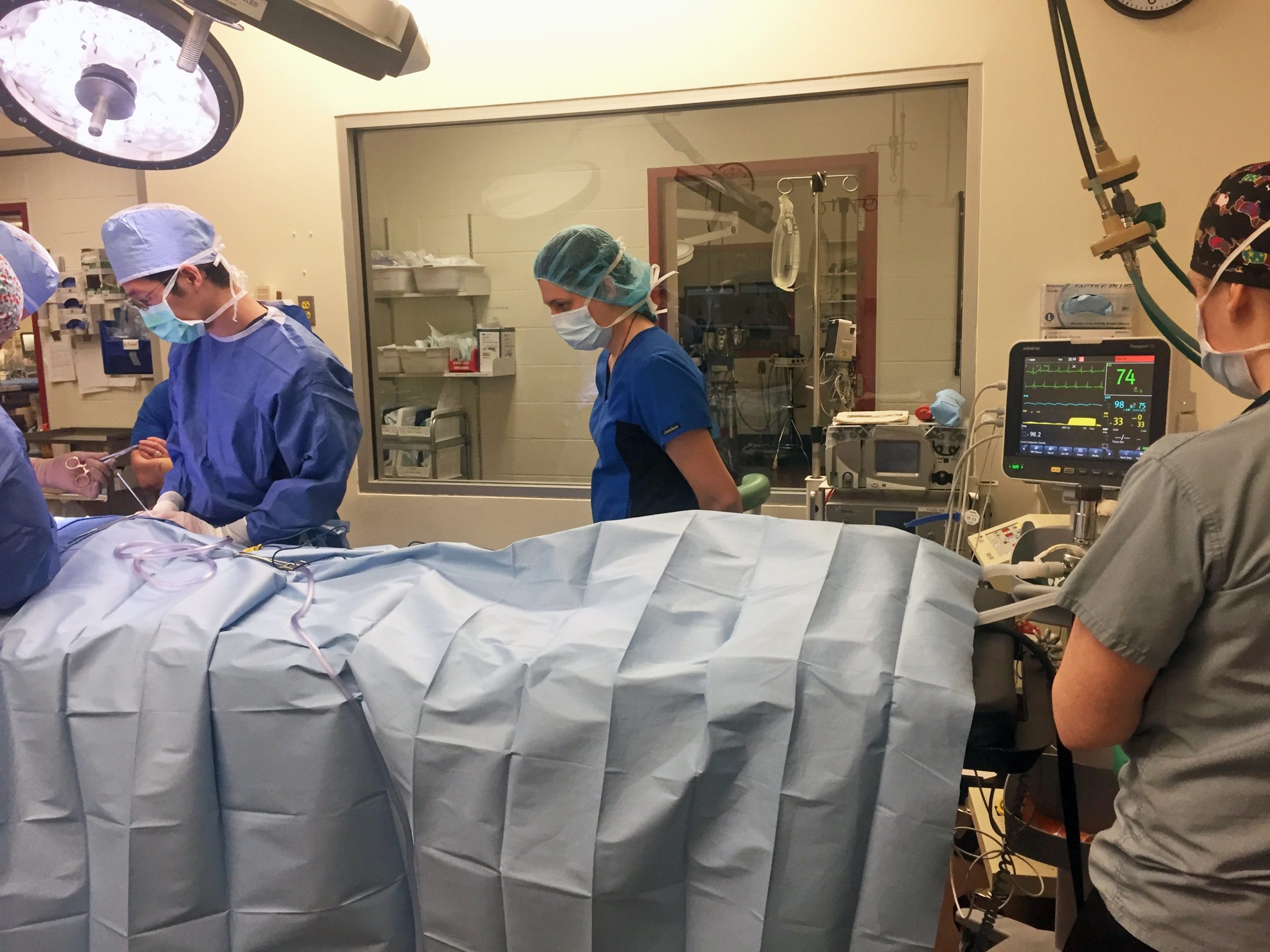
Lois Wetmore, DVM, MS, ScD, DACVAA: Number 1 is better monitoring. When I first started in veterinary anesthesia 30 years ago, we’d put an EKG on a dog during an operation to look at the electrical activity of the heart, attach a blood pressure cuff, and it was considered really good monitoring. The veterinary monitor that’s sold today checks blood pressure, heart rate, pulse oximetry, or oxygen saturation [what a physician is checking when she puts the little ‘clothespin’ on a person’s finger], body temperature, and capnography, which reflects how well the patient is breathing and whether carbon dioxide is being expelled from the body. This improved monitoring allows us to recognize better if the patient starts doing poorly and to make adjustments as needed. It’s called a multi-parameter monitor.
Your Dog: Do all veterinarians use a multi-parameter monitor when administering anesthesia?
Dr. Wetmore: I believe every veterinarian knows the importance of thoroughly monitoring their anesthetized patients and makes every effort to use monitors. Even for a small veterinary office, they tend not to be prohibitively expensive, running in the range of $4,000 to $8,000. It’s really important for the vet to have one because unlike in human medicine, there’s often not a person in the room dedicated to only overseeing anesthesia. The vet has to keep her eye on everything, and if she’s the one doing the surgery, it’s hard to pay attention to that and to the patient’s condition, but the monitor helps in that regard and can give a heads-up.
Your Dog: But isn’t there a veterinary technician in the room, which is like a veterinary nurse?
Dr. Wetmore: Often, yes. But we’re only at the start of veterinary technicians having specialty training, so relatively few veterinary technicians at this point have intensive schooling in how to recognize and treat problems of dogs under anesthesia. An anesthesiologist or a nurse anesthetist does not have to be in the room, as in human medicine. “Most practices rely heavily on the technicians receiving direction from the veterinarians to intervene when problems arise during anesthesia.
Your Dog: Gee, that doesn’t sound so good.
Dr. Wetmore: In a number of sub-specialties, orthopedics, for instance, veterinary medicine is on par with, or in some cases even ahead of, human medicine, at least when you’re talking about the skill and tools a board-certified veterinary orthopedist has on hand. That’s not the case with anesthesiology. As I indicated above, many of the operations in veterinarians’ offices are performed by general practitioners without a veterinary anesthesiologist present. That’s simply the current state of the art. In addition, human patients get a more detailed workup before an operation, so doctors for people have a better idea of what they’re getting into, what a patient’s particular needs and challenges might be with different anesthetic medicines. That’s part of the reason why, in veterinary medicine, problems arise during anesthesia for one in 1,000 to 2,000 patients, while for people it’s more like one in 100,000 patients.
Then, too, everything for veterinary anesthesiology is extrapolated from human medicine. When you have a teeny tiny 5-pound Yorkie and you’re trying to apply something used on infants in neonatal units, it can get tricky. Also, blood and fresh frozen plasma for transfusions are not as readily available in animal hospitals. Humans can get hundreds of units of blood transfused if need be. We don’t have 20 units of blood in the entire hospital, and many smaller practices don’t have any.
Your Dog: Why these gaps between human and veterinary medicine?
Dr. Wetmore: All of these issues — nurse anesthetists, equipment, pre-op workup, blood on hand — come down to money. The cost for anesthesiology is thousands of dollars for a person. With a dog, we can’t expect a client to pay that. So there’s relatively less intensive care. We are not ever going to be as good as human medicine when it comes to this. After an operation, a day in the intensive care unit for a person can run in the $50,000 range. In our ICU, it’s in the $400 range. There’s so much more available in human medicine than what we can afford to give our pets.
Your Dog: For people who love their dogs and want to do the best by them, this seems pretty dismal.
Dr. Wetmore: Dog owners can take heart. A complication rate of one in 2,000 —and it’s on the way to advancing to one in 10,000 — means your own pet undergoing anesthesia still has an extraordinarily slim chance of running into trouble. Let’s say if, during anesthesia, a problem arises. The doctor is taking out a tumor and there’s a lot of unanticipated bleeding. We have to be able to react to that: administer blood, plasma, platelets, other intraoperative support. We have these products now, and we actually can now recognize problems earlier and respond sooner with the better monitoring machines. And while a hospital might not have 100 units of blood, if it’s large enough it will at least have some. Moreover, more companies have opened up blood banks for dogs. It used to be that you had to keep a donor dog in your practice. Now, you can just call the blood bank, and they will deliver. Other improvements increase the odds for a good outcome, too.
Your Dog: Such as?
Dr. Wetmore: Well, historically, dogs going under anesthesia didn’t always have an IV catheter placed. If that line is not in, it’s harder to address problems that occur during an operation or other procedure by, say, administering drugs, fluids, even collecting blood for analysis during the procedure; you can’t easily change course in the middle. That could be very dangerous if the dog’s blood pressure drops and you need to very quickly give him a drug to bring it back up but don’t have the line as ready access.
Today, placing an IV catheter is considered standard practice. You can then give a drug “to effect” and so have less risk of overdose. Here at Tufts we are big advocates for it. But even here, we occasionally have to work without it because the pet is very fractious — it makes it hard to insert the line into a vein until we’ve already given them drugs to sedate them. That’s a problem for two reasons. One is that it makes it harder to do a physical exam on the dog, which helps predict how well he will react to anesthesia. In addition, that puts the sedative into the dog without the ability to respond quickly if he reacts poorly. Still, if we can quickly place a catheter after administering the sedatives but before too much time has passed, we can respond to any problems that occur.


Your Dog: Anything else that’s making anesthesia for dogs more consistently successful than it used to be?
Dr. Wetmore: Veterinary anesthetic drugs themselves are becoming safer. Let me rephrase that. As the saying goes, ‘there is no such thing as a safe anesthetic. There are only safe anesthetists.’ All anesthetics can still be poorly used, and patients can die as a result, so ‘safer anesthetic’ is something of a misnomer. But we now have ones that come with new advantages. Specifically, we have shorter-acting ones, and ones whose effects are more reversible should something go wrong. They actually have reversal agents that you can administer if you need to.
Another thing that improves safety, hypothetically, at least, is that we are returning to an old practice of using local anesthetic agents to help us. Many years ago, before we had good inhalants to help a dog drift off, we would use a lot of locals to make the patient not react. But then better inhalants became more popular, and the locals, pass. In the last eight to 10 years, however, there has been a full swing back to doing more peripheral nerve blocks — local anesthetic techniques. This is big in human medicine right now, too. The more locals you can apply directly at the site to block the pain stimulus, the easier it is to have minimal inhalant requirements. You can use just a little inhalant to hold them there while the locals do the rest of the work to keep the dog still.
Your Dog: Why would you want less of the inhalant to make the dog ‘fall sleep?’
Dr. Wetmore: The inhalant is critical. It’s not what reduces pain — it induces a loss of consciousness and thereby keeps the patient from moving, which you need a lot more often in veterinary medicine because dogs won’t sit still if you instruct them to. Unlike in human medicine, you need the inhalant anesthetic — the “general” — for dental work, for radiation, MRI, and a lot of other procedures. But by relying too heavily on inhalants you run the risk of the dog’s blood pressure dropping dangerously low. That’s one of the biggest issues with anesthesia, and why it’s so important to be able to inject fluids through a line, if need be.
What can happen with an inhalant is that the dog’s blood vessels dilate — it’s called vasodilation. That means blood doesn’t flow through the vessels with as much pressure, or force, as it should, and you run the risk that all the dog’s organs won’t be perfused with the blood they need. The patient could die. If you add fluid, you’re literally adding volume to the blood so that even though the blood vessels have widened, or relaxed, the extra volume will work to increase the pressure with which the blood flows, making sure it gets to all the body’s tissues in the way it should. As a side note, I should add that the different types of fluid we have now stay in the bloodstream longer — that’s a new development, only within the last 15 years.
But obviously, if you need less inhalant because you’re using more locals, all of this becomes less of an issue. When I was in school 30 years ago, often we relied solely on inhalants to keep an animal from moving and didn’t give a lot of analgesics — painkillers. The price we paid was low blood pressure.
Your Dog: So more actual pain killers are used with anesthesia now, not just the inhalant drug to render the dog unconscious?
Dr. Wetmore: Yes, it’s a big advance, and it’s not just about going back to locals.
Your Dog: What do you mean?
Dr. Wetmore: The inhalant will keep a dog still, but relying solely, or almost solely, on it is not a good way to work because during surgery, pain pathways will be activated with no inhibition of them while the patient is unconscious. So that paves the way for a lot of post-operative pain. Now, in addition to local anesthetics that have the added benefit of reducing the amount of inhalant, opioids — a class of painkillers by themselves — are a big part of what we use during a procedure. These can be administered very carefully, balancing their positive analgesic effects against their negative effect of slowing the heart rate. We use a combination of several drugs now, each in small amounts, to block the pain pathways while minimizing the overall negative effects. It’s a net gain because no one drug in too large a dose is causing a problem.
What it means is that it’s no longer this or that — heavy use of inhalants or locals and analgesics like opioids. It’s this and that to get the best outcome, both in terms of safety and post-operative pain.
Unfortunately, what we are able to use is influenced by the human market. There’s no “veterinary only” market. And that human market is starting to dry up for us in terms of opioids. Opioids are becoming less available for a number of reasons, not just for dogs but for people, too. [See “The Other Opioid Crisis” on pages 8 and 9.]
Your Dog: So is that actually taking the state of veterinary anesthesia backwards?
Dr. Wetmore: Well, it’s an issue. Drugs are being temporarily removed from the market and then may or may not come back. It makes veterinary medicine very hard to practice when you rely heavily on just one, or one protocol. Vets really need to be thinking on their toes right now and responding appropriately: ‘When one drug isn’t available, what can I use instead?’ It’s not clear what the impact is going to be over time.
Your Dog: That’s pretty discomfiting for people worried about their dog’s safety.
Dr. Wetmore: There’s no sugarcoating the fact that it’s a problem. But at the same time, we’ve achieved better and safer results with anesthesia even though we’re bringing a much less healthy population of dogs onto the operating table for anesthesia than we did in the past. In the past, we had mostly healthy animals getting straightforward, simple procedures, and we didn’t monitor them real closely and kind of got away with it. Today, clients are expecting more complicated procedures, which inevitably take us longer to perform. It’s not like in the old days, when vets performed a procedure very fast — 20 minutes — so dogs and other animals wouldn’t suffer the consequences of adverse anesthetic effects. With cancer treatment, hip replacements, and other involved operations, dogs are ‘under’ longer.
But even with that, we have been able to make, and so far maintain, great strides in safety. We even know now that, just like in human medicine, administering antibiotics at the time of an operation reduces the risk of infection that occurs with surgery, which in turn reduces the risk of serious complications, including death, after surgery. We will work to keep improving outcomes with today’s much better monitoring and also by making drug adaptations as we need to.