Tufts University has reportedly become the first veterinary facility in the U.S. to use a new treatment for speeding up wound healing in dogs and other pets. Called cold plasma therapy (or cold atmospheric plasma therapy), it appears to hasten the skin’s return to normal when it has been compromised by such things as cuts and wounds. It can also clear the crusting, scaling, inflammation, and eruptions that sometimes appear as the result of infections associated with allergies and other conditions. Cold plasma therapy has already been used in veterinary medicine in Europe for a few years. Tufts veterinary dermatologist Ramón Almela, DVM, learned about it while practicing in Germany before coming to the U.S. and has now brought it to the Tufts Cummings School of Veterinary Medicine.
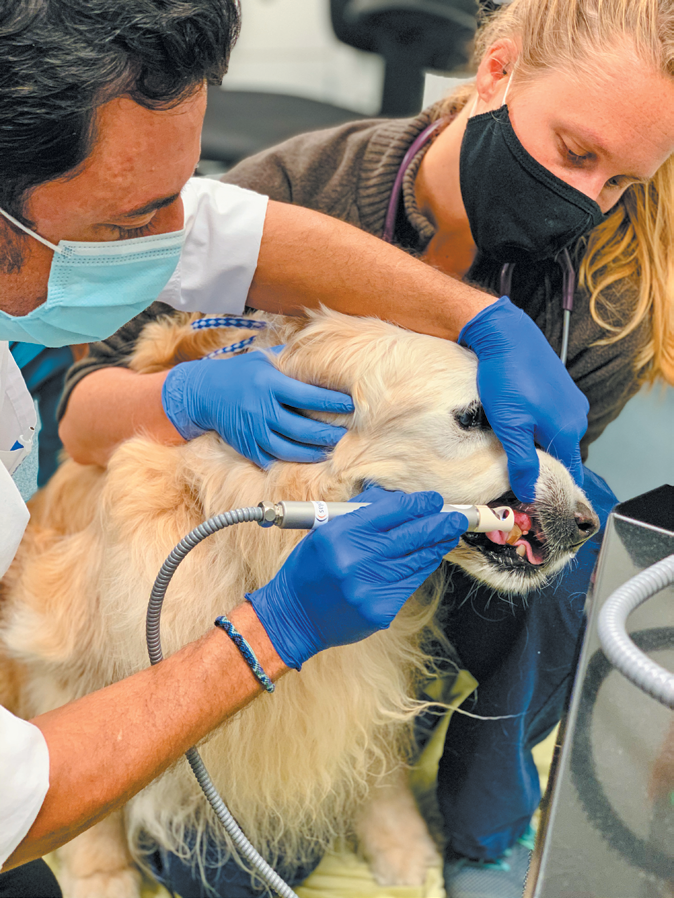
Dr. Almela’s first canine cold plasma patient stateside is a 16-year-old golden retriever named Melo. He had recurrent infections in his mouth around his upper right canine tooth that looked like “some type of bump or growth,” according to his owner, Rob Strasnick of Saugus, Massachusetts. “Something didn’t look right,” Mr. Strasnick says.
The default solution would have been to extract the tooth, but Mr. Strasnick and his wife did not want to put their 16-year-old pet through surgery and therefore were looking for another approach. That’s how they found Dr. Almela.
After twice-weekly cold plasma therapy treatments for a few weeks followed by once-weekly treatments for a few more weeks, the results seem clear. Dr. Almela reports that even pretty early on, there was less gum inflammation and less bleeding. And Mr. Strasnick says that “we have not had the bad breath that we attributed to the infection. And the white sore that was on the gum around the tooth has gone away and not come back.” In fact, Mr. Strasnick says, Melo “has been off antibiotics for a couple of months now, and the infection hasn’t returned.”
What is cold plasma therapy?
People think of matter as solid, liquid, or gas, but there is a fourth state: plasma. Plasma is what lightning is made of. “It’s somewhere between a gas and a liquid,” Dr. Almela says.
In the case of cold plasma therapy, a gas, usually argon, is turned into plasma. Then, aimed at a wound with the use of a small wand kept just off the body, the argon plasma is believed to regenerate healthy tissue via cell proliferation and angiogenesis — the creation of new blood vessels that nourish tissue.
At the same time that it promotes the growth of healthy cells, cold plasma therapy kills bacteria responsible for infections that can keep skin lesions from healing. Scientists and clinicians who are enthusiastic about the treatment believe it might even be an antidote to antibiotic resistance, which is the growing ability of harmful bacteria to resist antibiotics’ ability to kill them.
Research has suggested that the bacteria-killing ability of cold plasma therapy can help kill bacteria responsible for tooth decay, too — presumably a component of Melo’s problem. The plasma can easily coat crevices in the mouth that are difficult to reach with other dental decay-fighting mechanisms.
Scientific proof not yet nailed down
It must be noted that despite veterinarians’ clinical experience with cold plasma therapy and despite case studies reported in scientific journals, hard research on the procedure remains largely lacking in animals. In human medicine there are at least a few high-level studies comparing groups treated with cold plasma therapy to control groups. But there are very few studies published in peer-reviewed publications that take, say, two groups of dogs with similar skin wounds and compare their healing after giving one group standard treatment and the other, standard treatment plus cold plasma. In other words, the evidence in the veterinary field remains almost purely in the realm of anecdotal.
“A good analogy would be laser therapy,” Dr. Almela says. It is said to reduce the pain of such things as compromised joints, neurological problems, and fluid build-up that can reduce mobility, but there are no published studies of laser therapy in two groups of subjects proving that laser beams reduce pain more than standard pain treatments. Yet laser therapy is increasingly used in veterinary medicine, and veterinarians say they note a difference after laser applications.
“We need more hard evidence,” Dr. Almela says, “but the word of practicing clinicians is spreading.” Cold plasma therapy actually started with human medicine in Europe about 15 years ago.
Researchers are convinced enough of cold plasma therapy’s potential benefits that the Food and Drug Administration has recently approved its use in a clinical trial to see if it can eradicate remaining cancer cells after surgical removal of a malignant mass. The technology is expected to kill tumor cells by a mechanism similar to the way it kills harmful bacteria — by damaging malignant cells with the use of oxygen in the form of free radicals, which destroy diseased tissue.

Moving forward
No one is suggesting that cold plasma therapy should take the place of standard treatments for wound healing or allergies, including such tools as anti-inflammatory drugs, anti-inflammatory topical medicines, antibiotics, and flea treatments (even if the dog has not been shown definitively to be hosting fleas on its coat). In fact, part of Melo’s healing no doubt comes from the use of those medicinal tools.
Addtionally, the plasma does not penetrate deep into tissue. It can only be used for problems that are able to be treated superficially.
But both Melo’s owner, Mr. Strasnick, as well as Dr. Almela, believe the cold plasma therapy is giving the sweet-tempered dog’s wound healing a push. Better still, it’s completely safe — for the practitioner as well as the patient. “You don’t need special equipment — no glasses or ventilation,” notes Dr. Almela.
Moreover, the procedure is fast, about 30 seconds per square inch of affected skin, Dr. Almela says. And there is no need to sedate the animal because the treatment is painless. “The feeling is similar to a mild air flow,” he comments.