© AnnekaS | Bigstock


First the bad news. The geographic distribution of ticks that can infect dogs (and people) with Lyme disease is spreading. The Northeast has had the problem from the outset, and no area of the U.S. is completely Lyme disease-free, but the Companion Animal Parasite Control Council now says there’s going to be an increase this year, with Lyme disease making its way to areas that have not been of particular concern, like the Midwest and the Southeast.
Bird migration is part of it. Ticks carrying the Borrelia bacteria responsible for causing Lyme disease can migrate over large distances by bird travel. They then take hold in a new local area by attaching to deer and other wildlife, such as moose and a type of mouse called the white-footed deer mouse. Sometimes they don’t attach to the mice themselves but can lie in bedding that the mice prepare, and make their way from there onto dogs.
There’s also the issue of suburban sprawl. As housing developments and the countryside come smack up against each other, there’s more opportunity for ticks to make their way out of the woods and into peoples’ backyards and communities in general.
Finally, there’s climate change. Ticks become active when the temperature starts to approach 40 degrees Fahrenheit. And lately, in various areas of the country, the timing of seasonal changes can be more of a surprise. Says Mary Labato, DVM, a veterinary internist at the Tufts Cummings School of Veterinary Medicine and a member of our editorial advisory board, “this year, even in February in the heart of New England, we had 70-degree weather for a few days, and during that time, the ticks came out. We found a tick on my own dog in February. He ended up with anaplasmosis — a non-Lyme infection caused by a type of bacteria transmitted to dogs when ticks feed off them, resulting in clinical signs including fever, lethargy, and loss of appetite. These are similar to the signs of Lyme disease and have to be treated the same way — with a month-long course of antibiotics.
Bird migration, suburban sprawl, and climate changes were all highlighted as reasons for the uptick in Lyme disease in a new consensus statement published earlier this year by a distinguished group of veterinary researchers speaking on behalf of the American College of Veterinary Internal Medicine, or ACVIM. Among those researchers: Tufts’ own Dr. Labato. It is the first time since 2006 that information on the spread, diagnosis and treatment, and prevention of Lyme disease has been updated.
The good news from this group: Lyme disease is largely preventable — and treatable if your dog does become infected. Here’s what you need to know.
Effective steps for Lyme disease prevention
The ACVIM panel exhorts dog owners to follow a number of proven steps for protecting your dog from Lyme disease.
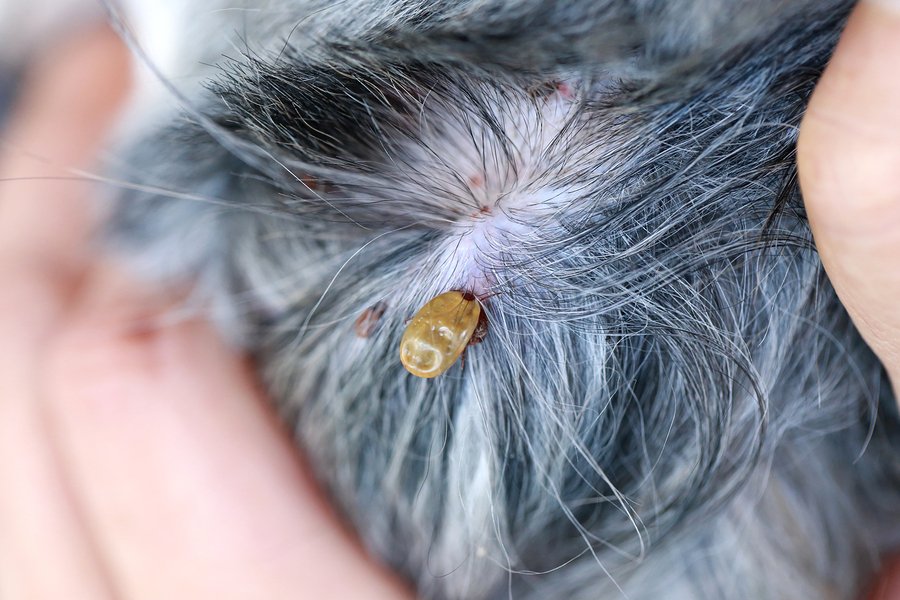
Routine checks for and removal of ticks. The consensus panel says unanimously that a first line of defense against Lyme disease in dogs is to conduct frequent checks for ticks and remove them as soon as they are identified. It is of “utmost importance,” they say, although they concede that it can be difficult in dogs with long or dark hair. That’s why the best approach is not only to look but also to feel your dog all along and around her back, tummy, limbs, face, and neck after you take her for walks in temperatures that are at least in the high 30s. A soft bump that has a texture something like a grape means the tick has started to feed off your dog and engorge, and the Lyme disease-causing bacteria can make their way from the insect’s gut into your pet’s bloodstream.
Don’t panic. Just immediately remove the tick with a special tick “rake” that you can buy at any pet goods store. Tweezers will do, too. Just be sure to grasp the tick right at the point of contact with your dog and lift up rather than side to side, retracting steadily. You have 36 to 48 hours from the time a tick attaches to your dog to the time your pet can become infected. It takes that long for a tick to pass the infectious agent from its saliva into your dog’s blood, which is what it feeds off of, Dr. Labato says. But other tick-borne diseases take hold faster, which is why you want to check for ticks every single day rather than every couple of days.
Exercise perimeter control. You can’t change the environment in parks or woods frequented by you and your dog, but you can make it more difficult for ticks to make their way onto your dog in your backyard. It’s just as important as checking your dog for ticks, says the new consensus statement, and that’s especially true if your dog regularly hangs out in the yard. Ticks really like living in underbrush and also are happy to jump onto your pet from long grass, so you can minimize chances for tick inhabitation both by keeping your lawn cut short along with cleaning areas of brush and weeds. In addition, use woods chips in gardens. They’re not ticks’ thing.
Those who use a fireplace or a wood-burning stove should be aware that bringing wood into the house can mean bringing in ticks. “Wood sheds are a nice place for ticks to take up residence over the winter,” Dr. Labato says. She also points out that in addition to wood piles, “piles of leaves and short shrubbery are ideal areas for ticks to hang out.” In the fall, don’t gather leaves from across the lawn and then leave them in a pile to remove another day. Take care of them the day you gather them.
Use a tick preventative year-round. The consensus among the panelists is strong that particularly in areas where tick-borne illness is endemic, a tick preventative should be used by conscientious pet owners year round not only to help prevent Lyme disease but also to prevent many other tick-borne diseases. The need remains just as strong even if your dog is given a Lyme disease vaccination because there are no vaccines for a number of other diseases that can infect a dog because of a tick bite.
A bevy of tick preventatives are available — collars, pills, and topicals — and “they all have their strengths and weaknesses,” Dr. Labato says, which is why you really need to talk to your vet about which is right for your dog in your particular area.
Chewables
Dr. Labato points out that there are three relatively new chewable drugs that have come out in the last few years: Nexgard, Simparica, and Brevecto. They all work not only against ticks but also fleas. They don’t prevent ticks from attaching to your dog, but the “kill” is relatively fast — less than 12 to 24 hours, Dr. Labato says, which means they also prevent tick-borne illnesses other than Lyme disease that can take hold more quickly.
All of the chewables are also good for dogs who go in the water a lot or get bathed often. You don’t have to worry that water will render the active ingredient ineffective, as can happen with some of the collars and also the topicals — definitely when you first apply them, and even between applications if your dog gets wet often. Nexgard and Simparica need to be given only once a month, Bravecto, every three months. Of course, some dogs will not take a tablet from you even if you wrap it in steak tartare and stand on your head.
MeePoohyaphoto | Bigstock

Topicals
For pill-averse dogs, there is also a Brevecto topical that needs to be rubbed between the dog’s shoulder blades every two months. In one study of Brevecto, the drug killed almost 90 percent of ticks after 4 hours, 98 percent by 8 hours, and 100 percent by 12 hours after application. A monthly topical called fiprinil, on the other hand (trade name Frontline), does not kill ticks until 24 hours after attachment. Drugs that kill faster are “preferred,” the panel says.
Four other topicals whose active ingredient is a drug called permethrin — Activyl T, Advantix II, Parastar, and Vectra 3D — are excellent in that they prevent tick attachment in the first place, but these drugs “should not be used on or near cats,” the panel says — important for owners of felines, as the active ingredient can cause severe and fatal poisoning even in cats who have simply come into contact with dogs who recently had the drug applied. (One name-brand topical, Revolution, does not kill the ticks responsible for Lyme disease and therefore is not recommended for tick control, the panel says.)
Note: Topicals are not the most effective route for dogs who frequently go into the water or are bathed often. Their efficacy will wane with frequent wetting, and a water-loving dog may need to be dosed more frequently.
Collars
Those who go the collar route, preferred by some because they only have to be changed every two to three months to every eight months, depending on the brand, should be aware that Preventic works only for ticks, not fleas. The Scalibor and Seresto brand collars, on the other hand, cover fleas, ticks, and mosquitoes. All the collars mentioned here prevent tick attachment, which is good, but like topicals, they preclude more than very infrequent swimming or bathing, and Preventic and Scalibor should not be worn by a dog in close proximity with cats. Tick collars should be applied tightly enough to have contact with your dog’s skin, not just her hair.
Testing, testing…
The panelists report that diagnosing Lyme disease has gotten easier because additional tests are now available to help rule out conditions whose symptoms mimic those of the Lyme infection. The tests also are better (but not perfect) at differentiating whether a rise in antibodies to the infectious agent is attributable to actual exposure to the offending bacteria because of a tick bite or simply because the dog was vaccinated against the bacteria and therefore has an increased antibody level in her blood.
They suggest that all dogs living in or near areas where Lyme disease is endemic get tested for antibodies to Lyme disease yearly as part of their annual wellness checks. This allows for prompt follow-up should there also be kidney values that are off (another potential sign of Lyme disease), and also provides an alert to people who live with other dogs, cats, or horses that the risk for exposure is elevated and extra precautions need to be taken.
The panelists do concede that the downside to testing all dogs in areas where Lyme disease is prevalent is the potential for the over-prescription of antibiotics. The fact is that most dogs infected with the bacteria responsible for Lyme disease and therefore having elevated antibodies to fight the illness never become ill because their immune systems are able to mount the necessary defense. That’s why four out of the six panelists do not routinely recommend antibiotic treatment for such dogs. In other words, according to the majority of the panel, elevated antibody levels themselves should not trigger a treatment regimen. But some veterinarians may prescribe antibiotics anyway to bring the antibody titers down — sometimes, because of anxiety on the part of dog owners who mistakenly fear that elevated antibodies automatically equate with illness.
Of course, there are dogs with elevated antibodies who do become ill from Lyme disease (in some cases evidenced by problematic kidney values), and all the panelists concur that in such cases, treatment is necessary.
If your dog does get sick
Despite the best of intentions and even good compliance with the steps for preventing Lyme disease, accidents happen, and dogs fall ill. Because ticks live outside and their life cycle takes place in concert with those of other animals along with environmental changes, it’s impossible to orchestrate complete immunity (although you can get close with good tick prevention compliance).
If your dog does end up with Lyme disease, the two most common manifestations of the illness are arthritis and kidney problems. (People — and horses — with Lyme disease often get neurological symptoms, but not dogs.)
The arthritis tends to present as lameness in a joint, or joints, accompanied by joint swelling, fever, and lethargy. Often, young, large-breed dogs with an active outdoor lifestyle are the victims, but no dog is immune. Fortunately, antibiotics take care of the problem, and dogs typically respond to them and start to feel better within a couple of days (although the dog should remain on antibiotics for a month).
The consensus panel recommends the antibiotic doxycycline as the first choice for most dogs with Lyme disease who have arthritic symptoms. It can work against infections that occur concurrently and is also purported to have anti-inflammatory properties that presumably could help reduce joint swelling.
Analgesics should be considered, too, to ratchet down a dog’s pain until her symptoms subside. One that your veterinarian might prescribe is gabapentin.
For dogs who end up with kidney problems, various drugs may be prescribed in addition to antibiotics — as well as dietary changes that include less protein and phosphorus and the addition of omega-3 fatty acids. For dogs whose kidney symptoms are severe, more drugs still will be added into the regimen. This is a more complicated problem than the arthritis.
Fortunately, far fewer Lyme disease-ridden dogs end up with kidney complications than with arthritic symptoms. And if you follow the guidelines for keeping ticks at bay, the odds became that much lower.
Should Your Dog Be Vaccinated Against Lyme Disease?
If you administer a tick preventative to your dog, you do not need to vaccinate her. The chewable, topical, or collar will do the trick. However, the panel notes that “compliance for using these products is an ongoing problem” — people don’t use them consistently — which is why many veterinarians, especially in places where the risk for Lyme disease is prevalent, recommend vaccinations as well. That said, the vaccinations do not work as effectively when used alone rather than in combination with tick preventatives. You’re not off the hook for using a tick preventative if you decide to get your dog inoculated.
Because of vaccinations’ only partial efficacy (and perhaps because vaccinations might provide a false sense of complete protection and lead people to mistakenly think they don’t need to use tick preventatives on their dogs if they inoculate), the six panelists on the ACVIM consensus committee were split down the middle on whether to recommend vaccinations for dogs living in areas with high Lyme disease rates; the vote was 50-50 rather than unanimous.
That said, no one on the panel was opposed to a Lyme vaccine for dogs. Dr. Labato says that “everyone felt the vaccines are probably safe and not likely to trigger kidney problems,” which had been a concern in the past.





